Pelvic Physiotherapy
The physiotherapists at our Nepean facility offer focused treatments and services for pelvic floor conditions, as well as prenatal and postpartum care, with a focus on women's health.
What is pelvic physiotherapy?
Pelvic physiotherapy is the assessment and treatment of conditions related to the pelvic floor and any symptoms that manifest themselves in that area. Pelvic Floor (Pelvic Health) Physiotherapists have additional postgraduate training that includes using internal and external manual techniques to evaluate pelvic floor muscle function.
We are proud to offer virtual physiotherapy appointments so that our clients can start or continue treatments from the comfort of home. If you prefer, our physiotherapists are happy to conduct your consultation virtually to discuss private or sensitive matters.
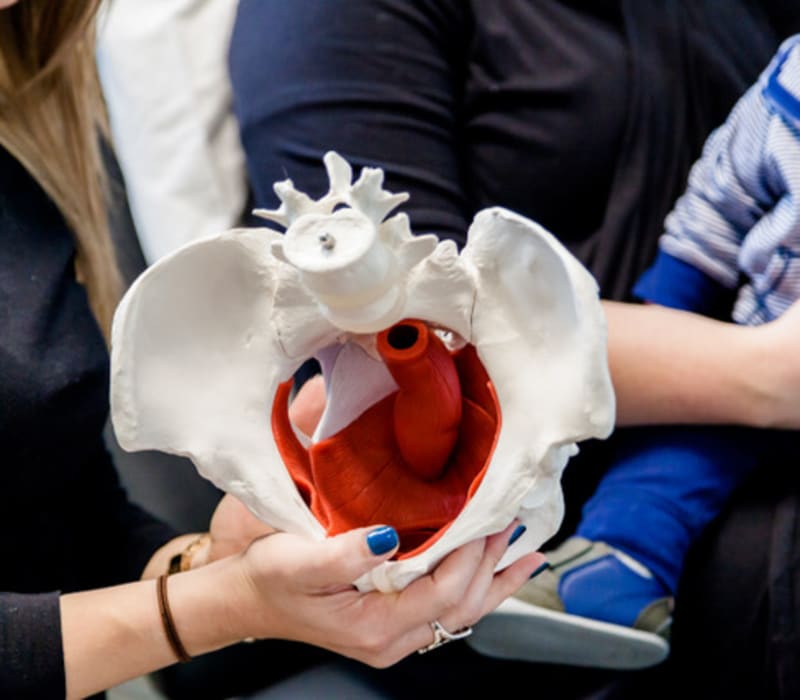
The Importance of the Pelvic Floor
The pelvic floor includes muscles, ligaments, nerves and connective tissue. The pelvic floor plays a critical role in the body, providing support for the abdominal and pelvic tissues and organs. It also helps with urine and bowel control and contains the muscles that contract during orgasm.
When the pelvic floor muscles become weakened, reduced bowel control and urine leakage can occur. For this reason, pelvic floor muscle training is very important, particularly for women after childbirth.
Although a healthy pelvic floor is integral to our health, many women (and men!) feel embarrassed to admit that they are suffering from pelvic floor dysfunction. As a result, it often goes untreated.
Silence on the subject results in a lot of unnecessary suffering – but it doesn't have to be that way!
Pelvic Health At Our Nepean Clinic
We want to help you feel comfortable when talking with us about your pelvic health. You don't need to feel embarrassed; we are here to help you!
The Pelvic Physiotherapist at Nepean Sports Medicine & Physiotherapy Centre is trained to provide internal assessment and pelvic health services.
We provide our pelvic physiotherapy services in a quiet, private treatment room.
We take care to provide a non-intimidating environment and make sure that our patients feel safe, comfortable and fully informed about their conditions and any related treatments.
-
Consultation
In our private treatment room, your physiotherapist will start by compiling a detailed history of your symptoms. They will ask you about the many other potential symptoms you may be experiencing that can go with pelvic floor dysfunction, such as sexual function, urine and fecal elimination, low back, hip and tailbone symptoms.
These questions may seem rather personal and unrelated, but if there are issues in any of these areas, they can often be related to pelvic floor dysfunction.
Your Pelvic Physiotherapist may also ask you to fill out a questionnaire in order to give her a better idea of what is contributing to your specific symptoms.
-
Assessment
Next, your Pelvic Physiotherapist will begin a series of physical assessments. The nature of these will depend on your symptoms, and may not all be completed on the first visit.
Your physiotherapist may assess your low back, SI joints, the connective tissue of the abdomen and thighs, and/or your pelvic floor itself.
A pelvic floor assessment is an internal exam that seeks to pin point trigger points in the pelvic floor, and assess the strength of the pelvic floor.
-
Treatment & Results
Your treatment will take place in a closed-door treatment room at our clinic that is solely dedicated to pelvic physiotherapy. Your comfort and privacy are our first concern.
Once your Pelvic Physiotherapist has completed the exam, they will discuss their findings with you.
They will give you exercises or other "homework" to do, and tell you when and how often you should return for treatment.
They will explain what changes you should expect to see, and how long you should expect your treatment to take.
They will give you time to ask questions.
Conditions That We Can Treat
Pelvic floor dysfunction and the conditions related to it are extremely common, but many people feel too embarrassed to seek help. The Pelvic Physiotherapist at our Nepean clinic can help you recover pelvic function and comfort.
-
Urgency
An intense and often sudden physical urge to urinate or defecate that can be difficult to control. This causes discomfort, and can make it difficult to delay using the toilet.
-
Vulvodynia
Chronic pain in the vulva.
-
Nocturia
If you find yourself waking up multiple times in the night to urinate, you may be suffering from Nocturia. Nocturia disrupts your sleep, and can be a sign of an underlying medical condition.
-
Constipation
Constipation is the difficult and infrequent passage of hard stools. If you are going for more than 3 days without a bowel movement, you may be suffering from constipation.
-
Frequency
Urinary Frequency is the need to urinate with a high frequency that disrupts your normal routine.
-
Incontinence
Incontinence is leakage of urine or feces that cannot be controlled. The severity ranges from occasionally urine leakage when coughing or sneezing, to an urge to urinate that's so sudden and strong you don't get to a toilet in time.
-
Chronic Pelvic Pain
Chronic pelvic pain can include any pain in or around the pelvic region that is present for three or more months with no physical diagnosis or medical explanation.
-
Pelvic organ prolapse
Pelvic organ prolapse is when one or more of the pelvic organs encroach on the vaginal space.
-
Interstitial Cystitis
Pain or burning with a filling, or full bladder, or upon emptying the bladder.
-
Vaginismus
A condition that affects a woman's ability to engage in vaginal penetration, such as sexual intercourse, insertion of tampons or menstrual cups, and the penetration during gynecological examinations (pap tests).
-
Dyspareunia
Difficult or painful sexual intercourse.
-
Coccydynia
Pain in the coccyx or tailbone area.
-
Persistent Low Back Pain
Pain in the low back that hasn’t been successfully treated with conventional physio.
-
Irritable Bowel Syndrome
A disorder that affects the large intestine.
-
Piriformis Syndrome
A condition in which the piriformis muscle, located in the buttock region, spasms and causes buttock pain. The piriformis muscle can also irritate the nearby sciatic nerve and cause pain, numbness and tingling along the back of the leg and into the foot.
-
Dysmenorrhea
Menstrual pain or cramps that occur before or during menstruation.
-
Pudendal Nerve Irritation (Alcock Canal Syndrome)
An uncommon source of chronic pain, in which the pudendal nerve (located in the pelvis) is entrapped or compressed.
-
Sciatica
Nerve pain from irritation of the sciatic nerve.
-
Symphysis Pubis
Dysfunctin pain at the pubic bone.
-
Sacroiliac Joint Dysfunction
Pain at the sacroiliac joint.
-
Diastasis rectus abdominis (DrA)
Separation of the rectus abdominus muscle, leading to a weakening of core function and strength.
-
Pregnancy-Related Body Pains
Such as low back, groin, pelvis pains, including carpal tunnel, water retention, and numbness/tingling related to pregnancy.
-
Endometriosis
A condition resulting from the appearance of endometrial tissue within the pelvic cavity causing pelvic pain.
-
Abdominal Surgery & Scar Tissue
If you have recently had surgery, or have scar tissue from a previous injury, a pelvic physiotherapist may be able to help you recover function and comfort.
-
Post Prostatectomy Incontinence
Loss of urine commonly experienced after prostate surgery.
-
Erectile Dysfunction
The inability of a man to maintain an erection.
-
Pain After Urination or Ejaculation
There are a variety of issues that could cause pain after urination and ejaculation in men, many of which can be treated with pelvic physiotherapy.
-
Groin Pain Due to Hernia Surgery
If you are suffering from groin pain after a hernia operation, a pelvic physiotherapist can help.
-
Testicular Pain
Testicular pain and pulling as a result of sexual dysfunction.
Pelvic Floor Physiotherapy FAQs
Read our pelvic health FAQs to learn about the conditions that can affect this area of the body, and what to expect from pelvic physiotherapy at Nepean Sports Medicine & Physiotherapy Centre.
-
What is the pelvic floor?
The pelvic floor is the muscular base of the abdomen, and is attached to the pelvis. It is made up of muscles, ligaments, nerves and connective tissue, and plays an important role in the body by providing support for the abdominal and pelvic tissues and organs.
-
What are some common conditions of the pelvic floor?
- Urgency: an strong physical urge to urinate or defecate that can be difficult to control.
- Nocturia: waking up at night with unusual frequency to urinate.
- Constipation: irregular and difficult passage of hard stools.
- Frequency: the need to urinate with a frequency that disrupts your normal routine.
- Incontinence: leakage of urine or feces that cannot be controlled.
- Chronic pelvic pain: pain in or around the pelvic region present for three or more months with no physical diagnosis or medical explanation.
-
What are some common treatments for pelvic floor complaints?
Depending on the variety and severity of your condition, your Pelvic Physiotherapist may employ different combinations of the following treatments:
Manual Therapy: Manual therapy is a range of hands-on techniques such as: soft tissue massage, mobilization, stretching, facilitation, as well as various trigger point release techniques.
Exercise & Stretching: A personalized exercise program will be designed for you by your physiotherapist. It will include a combination of strengthening exercises, stretches, good posture and breathing techniques, all of which are essential for good pelvic health.
Hypopressive Exercise: Hypopressive Exercises are specific breathing and posture techniques that decrease pressure to the abdomino-pelvic area, recruiting the pelvic floor muscles. These types of exercises can help prevent and treat urinary incontinence, prolapse conditions, and general posture.
Education: Understanding how various aspects of your lifestyle, diet, and urinary and bowel hygiene can affect your pelvic floor health, is important in maintaining it!
-
Is the internal examination really necessary?
An internal exam is the gold standard for assessment and treatment of pelvic floor conditions. Without feeling the muscles, your pelvic floor physiotherapist will be unable to identify if you have trigger points, or if you can contract your pelvic floor effectively.
That being said, there are many parts of the assessment and treatment that can be done without an internal exam. Some patients have been treated successfully without ever doing an exam.
Though the most benefit will be derived if your pelvic floor physiotherapist completes an internal exam, you will still benefit from pelvic physiotherapy if you are uncomfortable with or unable to have an internal exam. -
How many sessions are required?
This will depend on the type of condition you have, and its complexity. In general, for simple incontinence or prolapse (without any exacerbating factors), you will require 6-12 treatments. If you have a complex pain issue, this will likely take longer.
-
Is there homework to do between sessions?
Yes, there will be work for you to complete between sessions. Some examples of homework you may have include stretches, strengthening exercises or tracking things like elimination habits, diet, and fluid intake.
-
What if I already tried doing kegels and they didn’t work?
Pelvic floor physiotherapy involves much more than just kegels (pelvic floor muscle training). If you have tried doing kegels in the past but have not noticed any improvement, there could be many reasons, and you may need a different type of therapy or treatment.
Up to 30% of women are unable to do a kegel when asked. Many women instead contract their abdominals, glutes, or adductors. Or they bear down (push). If this is the issue, you may have been attempting to do kegels, but you have actually been strengthening the wrong muscles. A pelvic floor physiotherapist will check vaginally or rectally so they can actually feel your kegel, and teach you how to locate and contract your pelvic floor.
If you have been doing kegels with no effect, the problem may be that your pelvic floor is actually too tight, or has trigger points. For a muscle to be effective, it needs to have strength, but it also needs to be able to relax. For instance, if you can’t open your fist, strengthening your hand is not going to help. So in some cases, doing kegels may actually make your symptoms worse. Instead, your physiotherapist will release the tension or trigger points in your pelvic floor muscles, and give you stretches or other exercises to do at home. Your physiotherapist will also help you determine what other factors may be contributing to the tension or trigger points in your pelvic floor. -
What if I have my period? Should I cancel my appointment?
Your therapist can still assess and treat the pelvic floor if you have your period. It can actually be beneficial, as the pelvic floor muscles and pelvic organs can be affected by the hormonal fluctuations, especially if you notice a cyclical relationship to your problem. If you don't want to have your assessment during your period, the therapist can either proceed with the assessment or treatment externally or you can reschedule your appointment, provided you give 1 business day’s notice.
-
Is my physiotherapist specially trained to do an internal exam?
Yes. Our pelvic physiotherapist has undergone and continues to seek post graduate training to provide internal assessment and treatment services. The College of Physiotherapists of Ontario requires physiotherapists to be listed on the roster in order to perform internal assessments and treatments.
-
How should I prepare for my first appointment?
You will be sent some forms to collect relevant personal information about you and your medical history. Along with this, please bring any reports from special investigations or testing such as urodynamic or MRI reports. Don’t worry if you don’t have them, we can always request them from your MD at a later time.
You may bring a change of clothes to be most comfortable. There isn’t much to prepare for the internal assessment, you will be asked to undress from the waist down, we have gowns for you to change into, and you will always be draped to your comfort level. -
How long is the assessment and subsequent treatment sessions?
Your initial assessment is one on one in a private room. It will be approximately 60 minutes with your Pelvic Floor Physiotherapist. Follow up visits will be determined during your assessment, as they are catered to your particular needs but generally between 30 to 45 minutes per session. We highly recommend booking your appointments ahead to ensure your preferred time.
-
Can I bring my baby with me?
Yes. Your physiotherapist and our team welcome you to bring your baby with you for your appointment; you can even nurse during certain treatment techniques.
-
Will my extended health insurance cover pelvic floor physiotherapy?
Pelvic floor physiotherapy falls under the domain of physiotherapy, regardless of the area being treated. If you have insurance coverage for physiotherapy then pelvic floor physiotherapy will be included. But we encourage you to follow up with your insurance provider to confirm coverage. Please note that some insurance plans require a physician prescription in order to be reimbursed for physiotherapy services, even though you do not need a referral to see the Physiotherapist.
-
If I am pregnant, should I avoid an internal examination?
No, it is not necessary to avoid an internal examination when pregnant. If your doctor or midwife has not told you to avoid intercourse during pregnancy, an internal exam should be safe. If unsure, speak with your doctor or midwife directly prior to having an internal exam.
-
How long should I wait to have an internal exam after giving birth?
You should wait approximately 6-8 weeks after delivery before having an internal pelvic floor exam. This is true for vaginal deliveries and C-Section births. It is important to allow your body time to heal.However, many clients are choosing to set up a virtual post-baby checkup as early as 1-2 weeks after birth, to review breastfeeding, self-care, scar healing tips, and more!
During this time, you will also see spontaneous healing of a rectus diastasis, which should be checked at your follow-up appointment 6-8 weeks post-partum.
-
When is it unsafe to have an internal examination?
Internal examinations and treatments should be avoided if you have:
- Active hemorrhoids or infections
- Rectal bleeding
- Seed implants
- Radiation injuries less than 6-12 weeks old
- Undergone pelvic surgery less than 6 weeks ago
- Undergone prolapse repair surgery less than 12 weeks ago
- Been told by your doctor or midwife that you must abstain from intercourse or internal examinations during pregnancy
-
Is the internal exam similar to a gynecological exam?
Not really. Pelvic health physiotherapy is very different than an exam done by your physician or gynaecologist. We have much more time to do the assessment, and we do not use any big equipment (no speculum here!). Your physiotherapist will walk you through what they are doing every step of the way to make sure you are comfortable at all times.
-
Are there any risks to this treatment?
We create a private and sterile environment during assessment and treatment. We use a private treatment room, non-latex gloves and hypoallergenic gel, and wash or dispose of equipment properly. Your dignity and comfort is our highest priority.
There is a risk that you might feel some mild discomfort in the pelvic area after a treatment, particularly if it has involved stretching or trigger point massage to tight or tender muscles. Not all physiotherapists are certified to treat Pelvic Floor dysfunction. In order to perform internal examinations, your Physiotherapist has taken specific training, including a written certificate exam.
Interested in pelvic floor physiotherapy?
Our physiotherapists have focused training in the evaluation and treatment of pelvic floor dysfunction. We can address issues affecting anyone, including urinary and bowel control issues, pelvic pain, painful intercourse, pelvic organ prolapse, pre and postpartum issues, erectile dysfunction, and much more.
